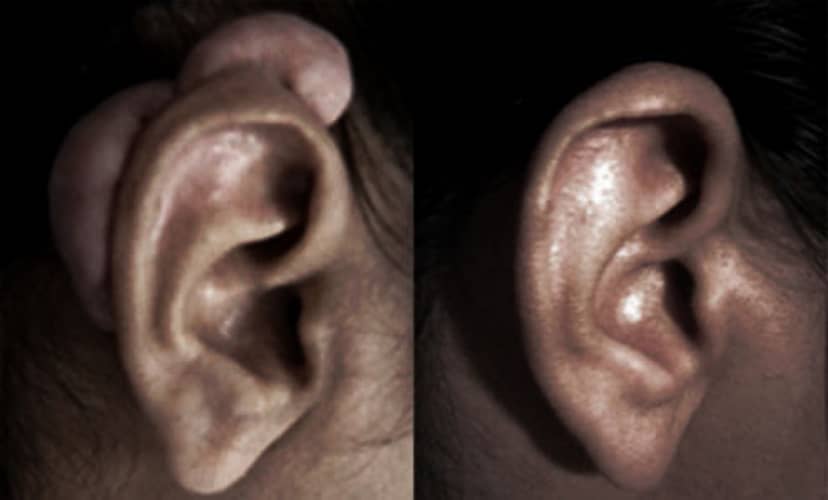
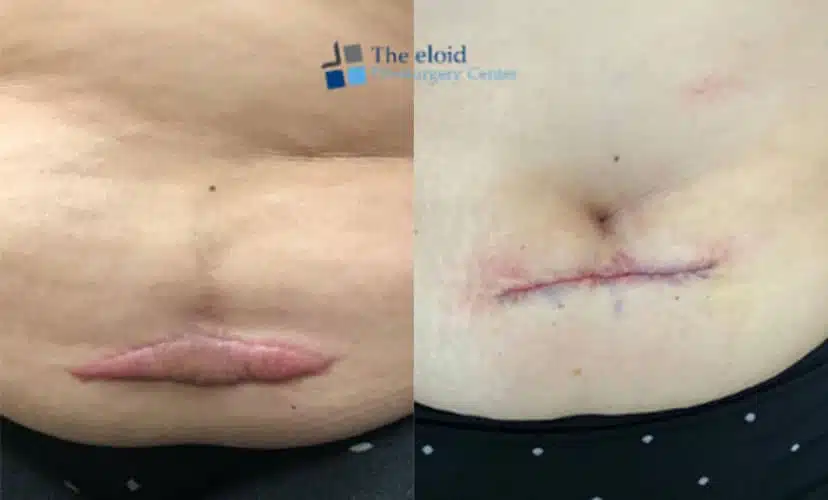
Have you ever wondered what happens during a keloid removal surgery, and what risks may come with it? A keloid is a fibrous and noticeable scar that develops after the skin heals from an injury, often due to an overproduction of collagen. While surgical removal can improve the appearance and discomfort associated with these scars, it also introduces important considerations such as recurrence, infection, delayed healing, and abnormal scar formation.
Because surgery creates a new wound, patients must understand not only how the procedure works, but also how the body may respond afterward. We’ll explore the different methods of keloid removal, the potential risks and complications associated with this surgical treatment, and the strategies used to minimize recurrence and promote safer results.

Understanding Keloids and Their Impact on Skin Health
- These scars can reduce skin elasticity and restrict movement, especially near joints.
- Keloids are raised scars caused by an overgrowth of collagen at the site of a healed skin injury.
- Although often considered cosmetic, keloids can also affect skin health and function.
- Some keloids cause symptoms such as discomfort, irritation, or persistent pain.
- Keloid formation results from an overactive healing response that disrupts normal skin repair.
Typical Treatment Options for Keloids
Various treatment options exist for patients with keloids. The primary approach is often therapy and using silicone sheets and gels. They help in flattening the keloids and reducing symptoms like itching and discomfort. Notably, steroid injections are a common treatment regimen, providing effective results by shrinking the keloids.
Another treatment involves using cryotherapy, a cold treatment that can reduce the size of keloids. Laser treatment is also a viable option, which can reduce the keloid’s redness and even help flatten the scar. Radiation therapy is another keloid removal procedure with a high success rate.
Patients must discuss these treatment options with a healthcare provider to determine a suitable choice. Keloid treatment is dependent on the size and location of the keloid and the level of symptoms experienced.
In some cases, surgical removal is recommended. However, surgery introduces new risks, including recurrence and complications, which must be carefully considered.
Delving into Keloid Scar Removal Surgery
Keloid surgical removal requires precise technique and careful planning. The procedure involves making an incision around the scar to remove the excessive tissue while preserving as much healthy skin as possible. Surgeons aim to minimize trauma to surrounding tissue to reduce the likelihood of abnormal healing.
Because surgery creates a new wound, it may trigger abnormal healing responses in some patients, increasing the risk of recurrence or abnormal scar formation.
Surgical Incisions in Keloid Removal
The incision process is a delicate balance between removing the keloid and preserving as much healthy skin as possible. The surgeon uses a scalpel to cut around the keloid tissue, aiming to excise it without causing unnecessary harm to the surrounding normal skin.
Role of Sutures in Ensuring Closure
After the keloid is removed, the incision must be closed securely to support proper healing. Sutures help approximate the skin edges and reduce tension across the wound, which is important in preventing abnormal scar formation.
Improper wound closure or excessive tension may contribute to abnormal healing and increase recurrence risk.
A Deeper Look at Surgical Excision
Surgical excision involves removing the entire keloid scar, often with a small margin of surrounding tissue to reduce the chance of residual abnormal cells. In some cases, reconstructive techniques such as a skin graft or local flap may be used to close the wound and improve cosmetic outcomes.
Despite complete removal, the body’s healing response may still trigger the formation of new keloids.
Leading Experts in Keloid Plastic
Surgery in Miami Beach

What Are the Main Risks of Keloid Removal Surgery
Keloid removal surgery can improve scar appearance and symptoms, but it also carries potential risks. Because the surgical procedure creates a new wound, the body’s healing response may sometimes lead to complications, especially in individuals prone to abnormal scar formation.
Recurrence of the keloid
Recurrence is the most common risk, as the skin may produce excessive collagen again during healing, causing the keloid to return at or near the surgical site.
Infection at the surgical site
Infection can occur if bacteria enter the wound, leading to redness, swelling, pain, warmth, or discharge, which may interfere with proper healing.
Hypertrophic scar formation
Some patients may develop a hypertrophic scar, which is a raised scar that remains within the surgical area but may still cause discomfort or cosmetic concerns.
Delayed wound healing
Slower healing can prolong inflammation and increase the risk of complications, particularly in areas with higher skin tension or reduced blood supply.
Changes in skin pigmentation
The treated area may become darker or lighter than the surrounding skin due to inflammation and disruption of normal pigment production during healing.
Why Keloids Can Return After Surgical Removal
Although surgery can remove the visible keloid scar, it does not eliminate the underlying tendency of the skin to form abnormal scar tissue. Keloids develop due to an overactive healing response, and surgical excision creates a new wound that may trigger excessive collagen production again.
Several factors increase the likelihood of recurrence, including genetic predisposition, high skin tension in certain areas such as the chest or shoulders, and persistent inflammation during healing. Larger or long-standing keloids may also have a higher chance of returning after removal.
Because of this risk, surgery is often combined with preventive treatments such as corticosteroid injections, silicone therapy, or other medical interventions designed to regulate the healing response and reduce the chance of new keloid formation.
Hypertrophic Scar Risks After Keloid Removal Surgery
Following keloid removal surgery, some patients may develop a hypertrophic scar, which is a raised scar that remains within the boundaries of the surgical incision. While different from keloids, hypertrophic scars still reflect an abnormal healing response.
Key risk factors include:
- Genetic predisposition, which increases the likelihood of abnormal scar formation
- Excessive tension on the surgical wound, which can stimulate excess collagen production
- Surgical location, especially high-tension areas such as the chest, shoulders, or joints
- Prolonged inflammation during healing, which can disrupt normal tissue repair
Although hypertrophic scars do not extend beyond the original wound like keloids, they may cause discomfort, cosmetic concerns, and indicate a higher sensitivity to abnormal scar formation.
BEFORE & AFTER GALLERY
Natural & Unparalleled Results
Post-Surgical Care and Its Role in Reducing Complications
After keloid removal surgery, proper care of the surgical site is essential for reducing the risk of complications. Because surgery creates a new wound, careful monitoring helps detect early signs of infection, inflammation, or abnormal healing.
Post-surgical care helps reduce the risk of:
- Infection, which can interfere with normal healing
- Excessive inflammation, which may trigger abnormal scar formation
- Recurrence, caused by an overactive healing response
- Pigmentation changes due to prolonged irritation or sun exposure
Following the surgeon’s instructions carefully helps stabilize healing and minimize complication risks.
Why Proper Skin Protection Helps Reduce Risk
Protecting the surgical area from excessive tension, irritation, and sun exposure helps reduce inflammation and supports controlled healing. Excessive irritation or ultraviolet exposure may increase the risk of abnormal pigmentation or scar recurrence.
Patients should follow their surgeon’s medical guidance to support safe healing and reduce complications.
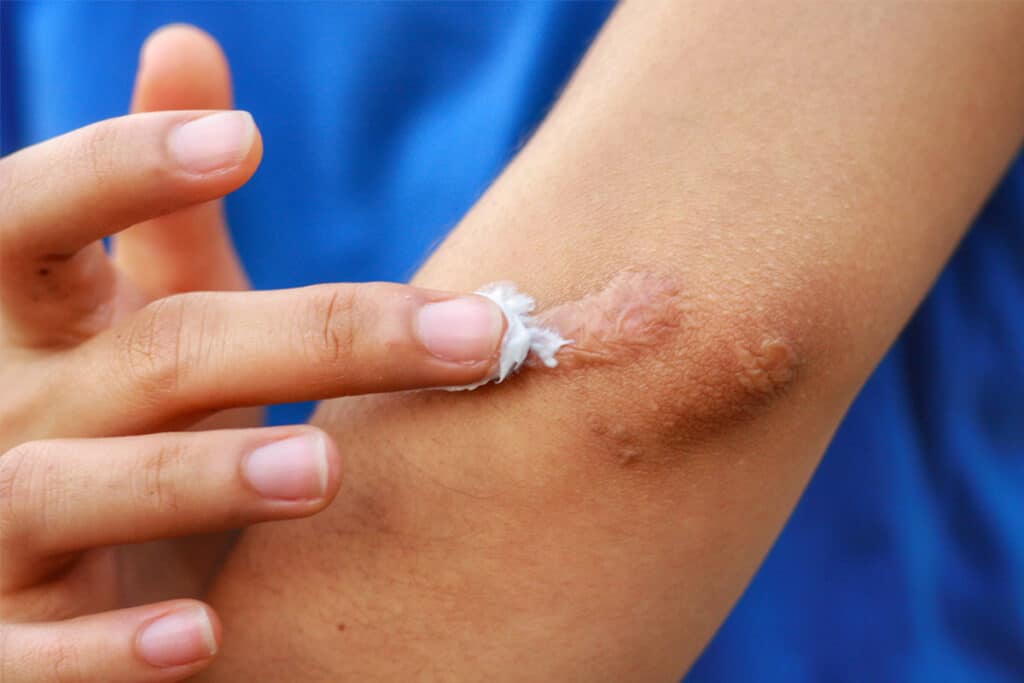
Healing Time After Keloid Removal Surgery and Its Impact on Risk
Healing time after keloid removal surgery varies depending on the size, location, and individual healing response. While many surgical wounds close within a few weeks, the internal healing process continues for several months.
Delayed or prolonged healing may increase the risk of complications, including infection, abnormal scar formation, or recurrence. Careful monitoring during this period allows early detection and management of potential complications.
Preventing Recurrence after Keloid Removal Surgery
Preventing the recurrence of keloids after removal surgery is one of the most important goals of keloid removal surgery. Because keloids result from an overactive healing response, additional treatments are often used to regulate collagen production and reduce risk.
Common preventive measures include:
- Corticosteroid injections to suppress excessive collagen production
- Silicone sheeting to stabilize healing and reduce scar activity
- Compression therapy to limit abnormal tissue growth
- Careful surgical techniques that minimize wound tension
These preventive strategies are essential because recurrence remains the most common complication following keloid removal surgery.
Steroid Injections and Their Role in Reducing Risk
Steroid injections are commonly used to reduce the risk of keloid recurrence after surgical removal. These injections help regulate the healing response by reducing inflammation and limiting excessive collagen production.
By controlling abnormal scar activity, steroid therapy lowers the likelihood of recurrence and improves surgical outcomes. However, treatment must be carefully managed by a qualified physician to ensure safety and effectiveness.
Choosing the Right Surgeon for Keloid Removal Surgery
Selecting an experienced surgeon is critical for minimizing surgical risks and improving long-term outcomes. Proper surgical technique, careful wound closure, and the use of preventive therapies can significantly reduce the likelihood of complications and recurrence.
An experienced specialist can evaluate individual risk factors, such as keloid size, location, and personal healing tendencies, to develop a treatment plan that promotes safer healing.
Schedule a Consultation for Keloid Scar Removal
If you or someone you know is living with keloid scars, we invite you to book an appointment with Dr. Salloum and Dr. Mendez. As experts in keloid removal, both plastic surgeons strive to provide safe procedures and minimize the risk of complications during surgery. With their extensive knowledge and personalized care, they will ensure that your keloid scar removal procedure is done correctly and efficiently. Don’t wait any longer, contact us today to learn more about our services.
Frequently Asked Questions About Keloid Removal Surgery Risks
Yes. Recurrence is the most common risk because the skin may produce excessive collagen again during healing.
Infection is uncommon but possible. Proper surgical technique and monitoring help reduce this risk.
In some cases, abnormal healing responses may cause recurrence or hypertrophic scar formation.
Patients with genetic predisposition, high skin tension areas, or previous keloids have a higher recurrence risk.